PATHOLOGIES
Mitochondrial diseases alone are quite rare but, if taken as a whole, they are the most common genetic diseases in humans with a prevalence of about 1 out of 5000 individuals in the European population. Clinical manifestations of mitochondrial diseases are mainly related to ATP production in organs and tissues, especially where and when energy need is high, and this is the case for nerve cells and muscle fibers.
This explains why mitochondrial disorders mainly involve CNS, skeletal muscle and heart.
However, mitochondrial pathology is, by definition, a multisistemic pathology involving many other tissues and / or organs such as liver, kidney, optic nerve, hematopoietic system, and endocrine system.
In childhood, clinical manifestations may include slowing or stopping of static-weight growth, psychomotor delay or regression, epilepsy, complex neurological signs, myopathy, optical atrophy and deafness.
Heart disease, hepatic disease, tubulopathy may also appear.
In neurological terms, different clinical phenotypes may be distinguished: Leigh syndrome, Leucoencephalopathy, poliodystrophy (often associated with hepatic disease, as in Alpers disease).
In adulthood, the most common symptoms are intolerance to the strain, weakness and muscle aches that appear after exercise, often in the form of cramps. Ocular motility disorders such as ptosis and / or ophthalmopenia are also quite frequent. Each of these conditions can be caused by alterations in several genes (see "Classification of Mitochondrial Diseases") and - in some cases - the same gene may be responsible for different phenotypes in the child and the adult (eg POLG).
When to suspect a mitochondrial disease
From what we said, it is evident that mitochondrial diseases have several clinical variables and, as a consequence, their diagnosis is difficult. Frequently, several specialists have to work together in order to reach a diagnosis: the neurologist, the pediatrician, the cardiologist, the lab physician, and the geneticist. Generally a mitochondrial disease must be suspected in all patients presenting a progressive imparement of both central and peripheral nervous system, together with the involvement of multiple organs that are not direclty related to each other.
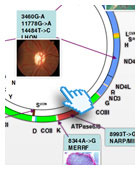
Typical morphological abnormalities found in muscle biopsy of patients affected by mitochondrial myopathy.
Morbidic map of mtDNA.
| Involved Organs | Possible correlated problems |
| Brain |
Psychomotor delay, dementia, epilepsy, psychiatric problems, migraine, stroke-like episodes. |
Peripheral nervous system |
Localized pain, deep reflexes absent, gastrointestinal disturbances (gastro-esophageal reflux, slow gastrointestinal movements, pseudo-obstruction), faintness and syncopal episodes, abnormalities of sweating, urinary bladder control and defecation. |
| Muscle | Hypotonia, muscle weakness with or without muscle wasting, exercise intolerance, cramps and myoglobinuria. |
| Kidney | Proximal tubular insufficiency (loss of proteins, magnesium, phosphorus, calcium, sodium, potassium and other important ions |
| Heart | Conduction defects, cardiomyopathy. |
| Liver | Hypoglycemia, liver failure. |
| Eyes | Visual loss, narrowing or other abnormalities of visual field. |
Auditory apparatus | Syndromic or non-syndromic, usually post-lingual, sensorineural hearing loss. |
Pancreas | Diabetes mellitus or insufficiency of exocrine pancreas leading to malabsorption. |
| Other | Failure to thrive, poor growth,short stature. |